Takayasu arteritis, often referred to as “pulseless disease,” is a rare, systemic inflammatory condition affecting the large and medium-sized arteries. It predominantly occurs in young Asian women and can lead to severe vascular complications if left untreated.
Introduction
What is Takayasu Arteritis?
Takayasu arteritis (TA) is a systemic inflammatory disease that causes damage to the large and medium arteries, including the aorta and its main branches. It is also known as “pulseless disease” due to the diminished or absent pulses in affected individuals. The condition primarily affects young women of Asian descent.
Epidemiology
- Incidence: TA is a rare disease with an incidence of 1 to 2 per million people globally.
- Demographics: The disease predominantly affects females, with a 9:1 female-to-male ratio.
- Age Group: It commonly occurs in individuals aged 40 to 50 years but can also be seen in children and the elderly.
- Geographic Distribution: Most prevalent in Asian and Mexican populations; rare in North America.
Etiology and Pathophysiology
Etiology
The exact cause of TA remains largely unknown. It is believed to be an autoimmune condition, where cell-mediated immunity plays a critical role. The inflammatory process leads to the thickening of arterial walls, resulting in stenosis, occlusions, or aneurysms.
Pathophysiology
- Inflammation: TA is characterized by granulomatous inflammation of the arterial walls, leading to fibrous thickening and vascular obstruction.
- Immune Response: CD4+ and CD8+ T cells are involved, supporting granuloma formation and activating proteases like matrix metalloproteinases (MMPs).
- Fibrosis: The disease leads to transmural fibrous thickening, causing multiple vascular obstructions and ischemic changes.
- Aneurysm Formation: Degeneration of elastic fibers and loss of medial smooth muscle cells can lead to aneurysm development.
Clinical Presentation
Early Symptoms
- Fever
- Malaise
- Weight loss
- Anorexia
- Muscle aches
Advanced Symptoms
- Hypertension: Due to renovascular stenosis.
- Neurological Manifestations: Resulting from carotid artery occlusion.
- Upper Limb Claudication: Due to upper extremity ischemia from arterial stenosis.
- Absent Pulses: A hallmark of the disease, leading to its nickname “pulseless disease.”
Evaluation
Diagnosis
- Clinical Suspicion: Based on history and physical examination.
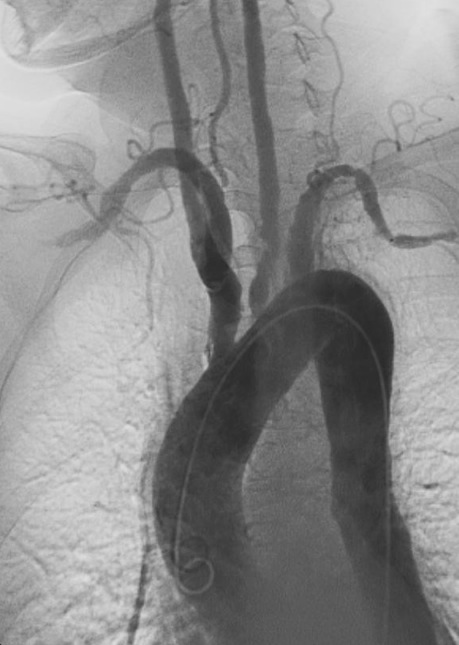
- Imaging:
- CTA (Computed Tomography Angiography): Preferred for initial staging and visualizing vessel wall thickening and luminal narrowing.
- MRI and MRA: Offer excellent multiplanar imaging without radiation but can overestimate stenosis.
Treatment and Management
Medical Management
- Corticosteroids: First-line treatment for reducing inflammation.
- Immunosuppressive Medications: Used in combination with corticosteroids, although their long-term efficacy is still debated.
Surgical Management
- Revascularization: Becoming a primary treatment option due to the high relapse rate with medical management alone.
- Transluminal Angioplasty: Offers short-term symptomatic relief but has high restenosis rates.
- Arterial Reconstruction: Involves using grafts like Dacron, PTFE, or autogenous saphenous vein, depending on the location and extent of arterial lesions.
Differential Diagnosis
- Aortic coarctation
- Atherosclerosis
- Behcet disease
- Giant cell arteritis
- Ig-G4 related disease
- Kawasaki disease
- Rheumatoid arthritis
- Sarcoidosis
Enhancing Healthcare Team Outcomes
Management of TA requires an interprofessional team approach, including:
- Specialists: Vascular surgeons, radiologists, cardiologists, internists, neurologists, and nephrologists.
- Nurses: Coordination of patient education and long-term monitoring for drug side effects.
- Pharmacists: Managing medication regimens and monitoring for adverse effects.
Conclusion
Takayasu arteritis is a complex vascular disorder requiring comprehensive evaluation and management. Early diagnosis and a multidisciplinary approach are crucial for improving patient outcomes. Long-term monitoring and treatment adjustments are necessary due to the potential for relapse and complications.
For further reading and self-assessment, access free multiple-choice questions on Takayasu arteritis through medical education resources.
References:
- Johnston SL, Lock RJ, Gompels MM. Takayasu arteritis: a review. J Clin Pathol. 2002 Jul;55(7):481-6.
- Arnaud L, Haroche J, Mathian A, Gorochov G, Amoura Z. Pathogenesis of Takayasu’s arteritis: a 2011 update. Autoimmun Rev. 2011 Nov;11(1):61-7.
- Mason JC. Surgical intervention and its role in Takayasu arteritis. Best Pract Res Clin Rheumatol. 2018 Feb;32(1):112-124.
- Comarmond C, Biard L, Lambert M, et al. Long-Term Outcomes and Prognostic Factors of Complications in Takayasu Arteritis: A Multicenter Study of 318 Patients. Circulation. 2017 Sep 19;136(12):1114-1122.

