Case Presentation
A 32-year-old male presents to the emergency department with severe chest pain, shortness of breath, and palpitations. He has a recent history of a viral upper respiratory infection but no significant past medical history.
History
- Chief Complaint: Severe, acute chest pain lasting several hours.
- History of Present Illness: The patient describes the chest pain as sharp and worsening with deep breaths. He also reports shortness of breath, palpitations, and fatigue. He had a viral upper respiratory infection about two weeks prior, characterized by fever, sore throat, and malaise.
- Past Medical History: No significant past medical conditions.
- Medications: No regular medications.
- Social History: Non-smoker, occasional alcohol use, no illicit drug use.
- Family History: No family history of heart disease or sudden cardiac death.
Physical Examination
- General Appearance: Mild distress due to pain.
- Vital Signs: Heart rate of 110 beats per minute, blood pressure of 130/85 mmHg, respiratory rate of 22 breaths per minute, and temperature of 37.5°C.
- Cardiovascular: Regular heart rhythm with distant heart sounds, no murmurs detected.
- Respiratory: Clear lung fields on auscultation.
- Abdominal: Soft, non-tender, no hepatosplenomegaly.
- Extremities: No edema, pulses are equal and strong bilaterally.
Initial Diagnostic Workup
Electrocardiogram (ECG)
The patient’s ECG reveals:
- Diffuse ST Segment Elevation: Seen in multiple leads, suggesting widespread myocardial involvement.
- T-Wave Inversions: Present in several leads, indicating myocardial inflammation.
- Sinus Rhythm: Heart rate is elevated at 76 beats per minute.
- No Pathological Q Waves: Absence of Q waves makes acute myocardial infarction less likely.
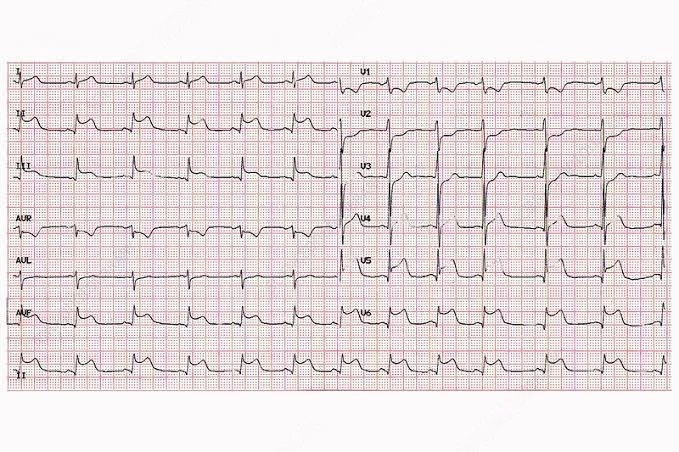
These findings support the possibility of myocarditis, especially in the context of a recent viral infection.
Chest X-Ray
The chest X-ray shows:
- Normal Cardiac Silhouette: No signs of cardiomegaly.
- Clear Lung Fields: No evidence of pulmonary edema or infection.
- No Pleural Effusion: Absence of fluid accumulation in the pleural space.
Laboratory Findings
- Cardiac Biomarkers:
- Troponin I: Elevated, indicating myocardial injury.
- CK-MB: Mildly elevated, consistent with cardiac muscle damage.
- Inflammatory Markers:
- C-Reactive Protein (CRP): Elevated, suggesting systemic inflammation.
- Erythrocyte Sedimentation Rate (ESR): Elevated, indicating ongoing inflammation.
- Complete Blood Count (CBC): Mild leukocytosis, supporting recent infection or inflammation.
- Viral Serologies: Positive for recent Coxsackievirus infection.
Echocardiogram
The echocardiogram shows:
- Mildly Reduced Left Ventricular Ejection Fraction (LVEF): Indicating some degree of ventricular dysfunction.
- Global Hypokinesia: Reduced movement across the heart muscle.
- No Significant Valvular Abnormalities: Valves appear structurally normal.
Cardiac MRI
The cardiac MRI provides detailed imaging of the heart:
- Diffuse Myocardial Edema: Consistent with acute inflammation.
- Late Gadolinium Enhancement (LGE): Indicates myocardial fibrosis and necrosis, characteristic of myocarditis.
Endomyocardial Biopsy
An endomyocardial biopsy is performed, revealing:
- Lymphocytic Infiltration: Presence of lymphocytes within the myocardium.
- Myocyte Necrosis: Evidence of myocardial cell death.
Diagnosis
Based on the patient’s history, clinical presentation, and comprehensive diagnostic workup, the diagnosis of viral myocarditis is established. The key factors leading to this diagnosis include:
- Recent history of viral infection.
- Diffuse ST segment elevation and T-wave inversions on ECG.
- Elevated cardiac biomarkers (troponin and CK-MB).
- Elevated inflammatory markers (CRP and ESR).
- Echocardiogram findings of reduced LVEF and global hypokinesia.
- Cardiac MRI showing myocardial edema and fibrosis.
- Biopsy confirming lymphocytic infiltration and myocyte necrosis.
What is Myocarditis?
Myocarditis is an inflammatory condition affecting the myocardium, the muscular layer of the heart. It disrupts the heart’s electrical system, leading to irregular heartbeats and reduced pumping efficiency. This condition can be triggered by various factors, most commonly viral infections, autoimmune diseases, and certain medications.
Causes of Myocarditis
- Viral Infections: Coxsackievirus, adenovirus, and parvovirus B19 are common culprits.
- Bacterial Infections: Although less common, bacteria like Streptococcus can cause myocarditis.
- Autoimmune Diseases: Conditions such as lupus and rheumatoid arthritis can trigger an immune response that attacks the heart.
- Medications and Toxins: Some drugs and toxins can induce myocarditis as a side effect.
Symptoms of Myocarditis
Symptoms vary widely, ranging from mild to severe. Common symptoms include:
- Chest Pain: Often mimicking a heart attack.
- Fatigue: Persistent tiredness even with minimal exertion.
- Shortness of Breath: Difficulty breathing, especially during physical activity or when lying down.
- Palpitations: Irregular or rapid heartbeats.
- Fainting: Syncope episodes due to heart arrhythmias.
Diagnosis of Myocarditis
Diagnosing myocarditis involves a combination of clinical evaluation, imaging studies, and sometimes biopsy.
Electrocardiogram (ECG) Changes
An ECG is a crucial diagnostic tool for myocarditis. The following ECG changes are commonly observed:
- ST Segment Elevation or Depression: Similar to those seen in myocardial infarction, these changes can indicate inflammation and injury to the heart muscle.
- T-Wave Inversions: These are common in various leads and reflect myocardial inflammation.
- Atrial or Ventricular Arrhythmias: Irregular heart rhythms, including premature ventricular contractions, atrial fibrillation, and ventricular tachycardia, may be present.
- Conduction Abnormalities: First-degree, second-degree (Mobitz type I and II), and third-degree atrioventricular (AV) blocks can occur due to the inflammatory process affecting the heart’s conduction pathways.
- Low Voltage QRS Complexes: These may be present, particularly in the setting of associated pericarditis or significant myocardial involvement.
- Diffuse ST Changes: Non-localized changes may be seen, reflecting a widespread inflammatory process.
Other Diagnostic Tools
- Echocardiogram (2D Echo): Uses ultrasound to assess heart function and structure.
- Cardiac MRI: Provides detailed images of the heart, revealing inflammation and damage.
- Blood Tests: Measure markers of inflammation and heart damage, such as troponin.
- Endomyocardial Biopsy: In certain cases, a small tissue sample from the heart is analyzed.
Treatment:
Treatment depends on the underlying cause and severity of the condition. The primary goals are to manage symptoms and reduce inflammation.
- Medications: Anti-inflammatory drugs, beta-blockers, and ACE inhibitors are commonly used.
- Lifestyle Modifications: Rest and avoiding strenuous activities are crucial during recovery.
- Treating Underlying Conditions: Addressing infections or autoimmune diseases is essential.
- Advanced Therapies: In severe cases, mechanical support or even heart transplantation might be necessary.
Prognosis and Complications
The prognosis for myocarditis varies. While some individuals recover completely, others may develop chronic heart conditions such as dilated cardiomyopathy or heart failure. Early detection and treatment significantly improve outcomes.
Conclusion
Myocarditis is a complex condition with potentially serious outcomes. Awareness of its symptoms, prompt diagnosis, and appropriate treatment are critical. Healthcare professionals must consider myocarditis in patients presenting with chest pain and a recent history of viral infection, as timely intervention can prevent severe complications.
Read more: