History
A 55-year-old male presents to the emergency department with sudden onset of shortness of breath, chest pain, and a history of recent immobilization following orthopedic surgery. The chest pain is pleuritic in nature, worsened by breathing and coughing. The patient also reports a history of deep vein thrombosis (DVT) and has been non-compliant with anticoagulant therapy.
Examination
On physical examination, the patient appears distressed and tachypneic. Key findings include:
- Vital Signs: Heart rate of 102 beats per minute (tachycardia), respiratory rate of 24 breaths per minute, blood pressure of 100/70 mmHg, and oxygen saturation of 88% on room air.
- Inspection: Cyanosis of lips and nail beds.
- Palpation: Tenderness in the left calf, suggestive of DVT.
- Auscultation: Clear lung fields with no signs of consolidation, but reduced breath sounds in the right lower lung zone.
Diagnostic Workup
ECG Findings
An electrocardiogram (ECG) is performed, showing:
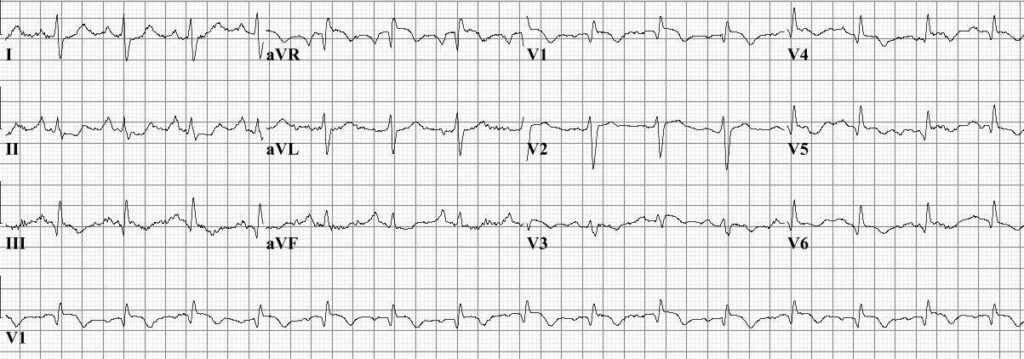
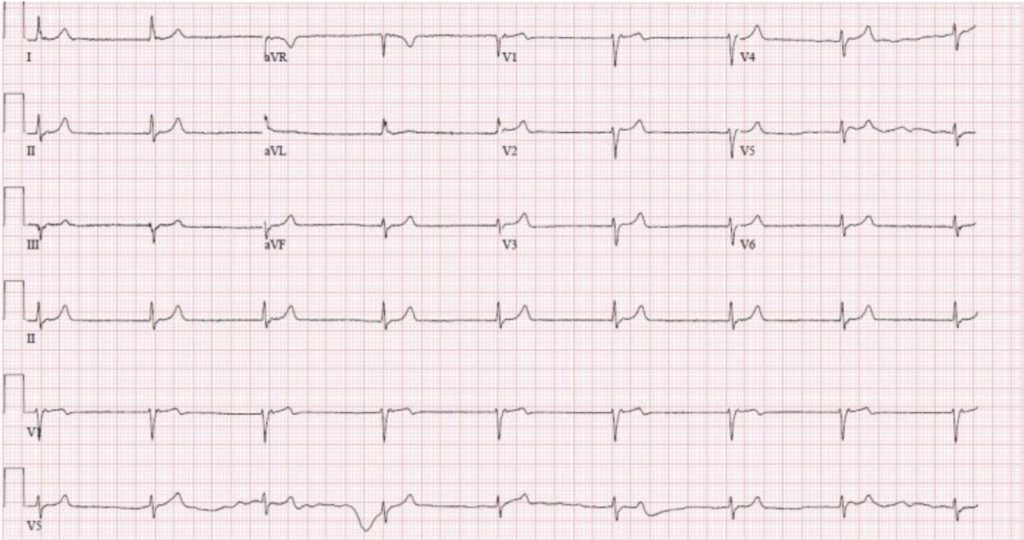
- Sinus tachycardia
- S1Q3T3 pattern: Deep S wave in lead I, Q wave in lead III, and inverted T wave in lead III, which can be suggestive of PE.
- Right axis deviation and right ventricular strain pattern.
Laboratory Tests
Blood tests reveal:
- D-dimer: Elevated, indicating the presence of an abnormal blood clotting process.
- Arterial Blood Gas (ABG): Hypoxemia with a PaO2 of 60 mmHg, and a slight respiratory alkalosis.
- Complete Blood Count (CBC): Mild leukocytosis.
- Troponin and BNP: Slightly elevated, indicating possible right ventricular strain.
Imaging Studies
Chest X-ray
A chest X-ray is performed but is largely unremarkable, which is common in PE. It helps to rule out other causes of chest pain and dyspnea.
CT Pulmonary Angiography (CTPA)
CTPA is the gold standard for diagnosing PE and shows:
- Filling defects in the right pulmonary artery and segmental branches, confirming the presence of a PE.
Additional Tests
Ultrasound of the Lower Extremities
A Doppler ultrasound of the legs shows:
- A non-compressible vein in the left calf, confirming the presence of a DVT.
Diagnosis
Based on the clinical presentation, physical examination, ECG findings, elevated D-dimer levels, and confirmatory imaging studies, the diagnosis of acute pulmonary embolism is established.
Management
Initial Stabilization
- Oxygen Therapy: To maintain adequate oxygen saturation.
- Intravenous Fluids: To maintain blood pressure and ensure proper perfusion.
Anticoagulation
Immediate anticoagulation is crucial to prevent further clot formation. Options include:
- Low Molecular Weight Heparin (LMWH): Administered subcutaneously.
- Unfractionated Heparin: Administered intravenously, particularly in hemodynamically unstable patients.
Thrombolytic Therapy
Considered in patients with massive PE and hemodynamic instability:
- Alteplase: A tissue plasminogen activator (tPA) can be administered to dissolve the clot.
Long-term Anticoagulation
After initial stabilization, patients are transitioned to long-term anticoagulation therapy to prevent recurrence:
- Warfarin: Requires regular monitoring of INR.
- Direct Oral Anticoagulants (DOACs): Such as rivaroxaban or apixaban, which do not require regular monitoring.
Supportive Measures
- Analgesia: To manage pleuritic chest pain.
- Compression Stockings: To prevent recurrence of DVT.
Conclusion
Pulmonary embolism is a medical emergency that requires prompt recognition and treatment. A systematic approach, including a thorough history, physical examination, appropriate diagnostic tests, and timely management, is essential for improving patient outcomes and reducing the risk of complications.