History
A 45-year-old woman presents to the emergency department with complaints of a severe headache, confusion, and visual disturbances that began suddenly. She has a history of hypertension, which is poorly controlled, and was recently diagnosed with systemic lupus erythematosus. She denies any recent head trauma or infections. Her medication regimen includes prednisone and antihypertensive drugs.
Examination
On examination, the patient appears disoriented and agitated. Vital signs reveal a blood pressure of 210/120 mmHg, indicating hypertensive urgency. Neurological examination shows bilateral papilledema, suggesting raised intracranial pressure. Reflexes are brisk, but there are no focal neurological deficits.
Laboratory Tests
Initial laboratory tests reveal the following:
- Complete Blood Count (CBC): Normal white blood cell count, hemoglobin, and platelet levels.
- Electrolytes: Sodium and potassium levels within normal limits.
- Renal Function: Elevated serum creatinine, indicating renal impairment.
- Autoimmune Panel: Positive for anti-nuclear antibodies (ANA) and anti-dsDNA, consistent with lupus.
Imaging Studies
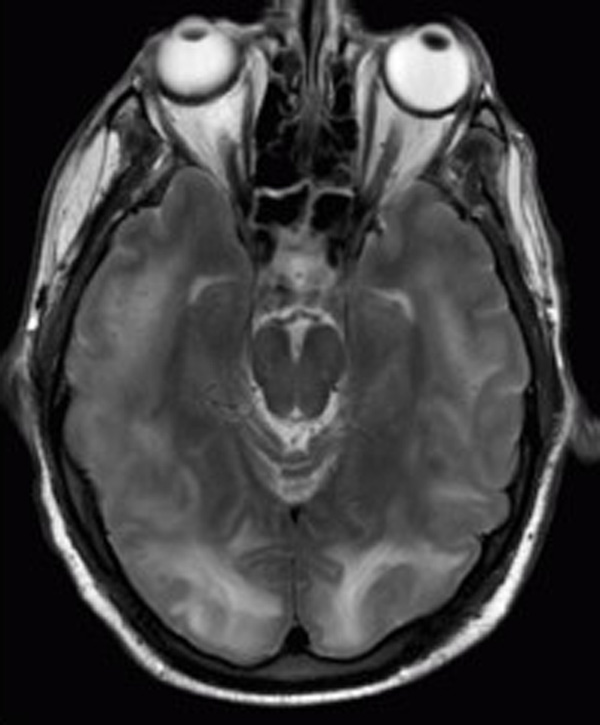
Magnetic Resonance Imaging (MRI) of the brain is performed, revealing hyperintense lesions in the parieto-occipital regions on T2-weighted and FLAIR sequences. These findings are suggestive of vasogenic edema, a hallmark of PRES.
Diagnosis
Based on the clinical presentation, history of hypertension and autoimmune disease, and characteristic MRI findings, the diagnosis of PRES is made. The condition is confirmed by ruling out other potential causes of similar symptoms, such as infectious encephalitis or acute demyelinating diseases.
Overview:
Posterior Reversible Encephalopathy Syndrome (PRES) is a neurological disorder characterized by a range of clinical and radiological findings. It presents with symptoms such as headache, altered mental status, seizures, and visual disturbances. Despite its name, PRES can affect regions beyond the posterior part of the brain, and while often reversible, it requires prompt recognition and treatment to avoid permanent damage.
Pathophysiology
PRES is thought to result from a failure of cerebral autoregulation due to severe hypertension or endothelial dysfunction. This leads to leakage of fluid into the brain parenchyma, causing vasogenic edema. The posterior circulation is particularly vulnerable due to its less effective sympathetic innervation.
Management and Treatment
Immediate Management
The primary goal in managing PRES is to control blood pressure. In this case, the patient is administered intravenous antihypertensive agents to rapidly reduce blood pressure to safer levels. Additionally, seizures are managed with antiepileptic medications.
Supportive Care
Supportive care includes:
- Monitoring and maintaining electrolyte balance.
- Ensuring adequate renal function.
- Regular neurological assessments to track improvement or deterioration.
Long-Term Management
Once the acute episode is managed, long-term strategies focus on:
- Blood Pressure Control: Adjusting antihypertensive medications to prevent future hypertensive crises.
- Autoimmune Disease Management: Optimizing the treatment for lupus to prevent exacerbations that could trigger PRES.
- Follow-Up Imaging: Repeating MRI after a few weeks to ensure resolution of vasogenic edema and to check for any residual effects.
Prognosis
PRES typically has a favorable prognosis if promptly recognized and treated. Most patients recover fully within days to weeks. However, delays in diagnosis and treatment can lead to irreversible brain damage or death.
Conclusion
PRES is a potentially reversible but serious condition that requires quick and effective intervention. Awareness and understanding of its presentation, diagnostic criteria, and management strategies are crucial for improving patient outcomes. Regular follow-up and control of underlying conditions are essential to prevent recurrence.