Shingles
Shingles, a viral infection characterized by a painful rash, is caused by the varicella-zoster virus, the same virus responsible for chickenpox. Despite being a dormant virus in those who have had chickenpox, it can reactivate years later, leading to the development of shingles.
What is Shingles?
Shingles, also known as herpes zoster, manifests as a painful rash typically occurring on one side of the body. The rash typically forms a band or stripe pattern along a nerve pathway and is often accompanied by sensations of burning, tingling, or itching. While anyone who has had chickenpox can develop shingles, the risk increases with age, weakened immune system, and stress.
Causes of Shingles
1. Varicella-Zoster Virus (VZV) Infection:
- Shingles is caused by the reactivation of the varicella-zoster virus, the same virus responsible for chickenpox.
- After a person recovers from chickenpox, the virus remains dormant in nerve tissue near the spinal cord and brain.
2. Reactivation of Dormant Virus:
- The varicella-zoster virus can reactivate years or decades later, leading to shingles.
- The exact trigger for reactivation is not fully understood but may be related to age, stress, or a weakened immune system.
3. Weakened Immune Response:
- A weakened immune system can fail to keep the virus in check, allowing it to reactivate and cause shingles.
- Conditions such as HIV/AIDS, cancer, or certain medications that suppress the immune system increase the risk of reactivation.
4. Age-Related Factors:
- Advancing age is a significant risk factor for shingles due to age-related changes in the immune system.
- As people get older, their immune response weakens, making them more susceptible to viral reactivation.
5. Nerve Damage or Irritation:
- Nerve damage or irritation can trigger the reactivation of the varicella-zoster virus.
- Trauma, injury, or surgery near nerve pathways may disrupt nerve function and facilitate viral reactivation.
6. Stress and Hormonal Changes:
- High levels of stress can weaken the immune system, making individuals more susceptible to shingles.
- Hormonal changes, such as those occurring during pregnancy or menopause, may also increase the risk of viral reactivation.
7. Immunosuppressive Therapies:
- Medications or treatments that suppress the immune system, such as chemotherapy or long-term corticosteroid use, can increase the risk of shingles.
- These therapies prevent the body from effectively controlling viral reactivation.
8. Genetic Factors:
- There may be genetic predispositions that influence the likelihood of developing shingles.
- Family history of shingles or certain genetic markers may indicate an increased risk for individuals.
9. Environmental Factors:
- Environmental factors such as ultraviolet (UV) radiation from sunlight may play a role in triggering viral reactivation.
- However, the exact contribution of environmental factors to shingles development is not fully understood.
10. Unknown Triggers:
- In some cases, the exact trigger for viral reactivation and the development of shingles remain unknown.
- Research continues to explore potential factors contributing to the onset of Herpes Zoster.
Signs and Symptoms :
1. Prodromal Symptoms:
- Before the rash appears, some individuals may experience prodromal symptoms, including:
- Pain, burning, or tingling sensation in a specific area of the skin
- Itching or numbness
- Fever or chills
- Headache
- Fatigue or malaise
2. Rash:
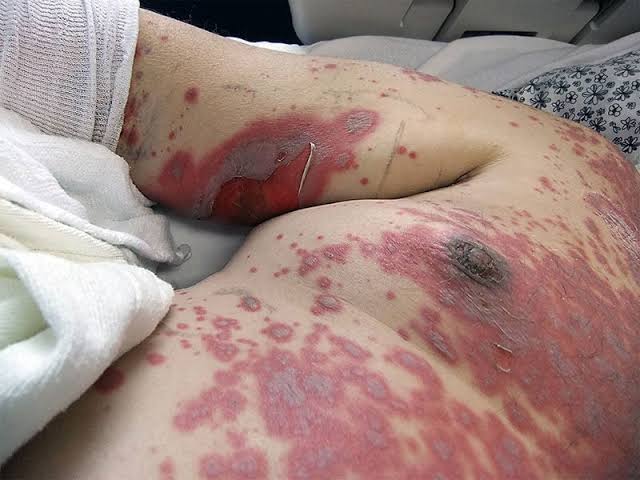
- The hallmark sign of shingles is a painful, blistering rash that typically appears on one side of the body or face.
- The rash usually begins as red patches of skin, which then develop into clusters of fluid-filled blisters.
- Over the course of 7 to 10 days, the blisters may burst, crust over, and eventually heal.
3. Unilateral Distribution:
- The rash typically follows a unilateral (one-sided) distribution pattern, confined to a specific dermatome—a region of skin supplied by a single spinal nerve.
- Common sites of involvement include the torso (chest or abdomen), face (including the eye area), neck, or back.
4. Pain and Sensitivity:
- Pain is a prominent symptom of shingles and often precedes the appearance of the rash.
- The pain may range from mild to severe and can be described as burning, stabbing, or shooting.
- Affected areas of the skin may also be hypersensitive to touch, temperature changes, or clothing.
5. Itching and Discomfort:
- In addition to pain, individuals with Herpes Zoster may experience itching, tingling, or discomfort in the affected area.
- Itching may intensify as the rash progresses and blisters develop.
6. Flu-Like Symptoms:
- Some individuals may experience flu-like symptoms along with the rash, including:
- Fever
- Headache
- Fatigue
- Muscle aches
7. Ophthalmic Involvement:
- When Herpes Zoster affects the eye (herpes zoster ophthalmicus), symptoms may include:
- Eye pain
- Redness and swelling of the eyelids
- Blurred vision or sensitivity to light
- Eye discharge
8. Neurological Complications:
- In severe cases, Herpes Zoster can lead to neurological complications such as:
- Postherpetic neuralgia (persistent nerve pain after the rash has healed)
- Facial paralysis (if Herpes Zoster affects the facial nerve)
- Meningitis or encephalitis (inflammation of the brain or spinal cord)
9. Immunocompromised Individuals:
- People with weakened immune systems may experience atypical or more severe symptoms of Herpes Zoster.
- The rash may be more extensive and widespread, and complications may occur more frequently.
10. Duration of Symptoms:
The duration and severity of shingles symptoms can vary widely from person to person.In most cases, symptoms resolve within 2 to 4 weeks, but pain or complications such as postherpetic neuralgia may persist for months or even years in some individuals.
Who get’s shingles? Risk Factors :
1. Age:
- Shingles primarily affects older adults, with the risk increasing significantly after the age of 50.
- The likelihood of developing shingles also rises with advancing age.
2. Weakened Immune System:
- Individuals with weakened immune systems due to conditions such as HIV/AIDS, cancer, or certain medications (e.g., corticosteroids) are at higher risk.
- Immunosuppressive therapies can increase susceptibility to Herpes Zoster.
3. Previous Chickenpox Infection:
- Shingles is caused by the reactivation of the varicella-zoster virus, the same virus responsible for chickenpox.
- Those who have had chickenpox in the past are at risk of developing shingles later in life.
4. Stress:
- High levels of stress can weaken the immune system, making individuals more susceptible to Herpes Zoster.
- Emotional stress, trauma, or physical stressors can trigger the reactivation of the virus.
5. Certain Medical Conditions:
- Conditions such as diabetes and autoimmune diseases may increase the risk of shingles.
- Chronic illnesses that compromise the immune system can elevate susceptibility.
6. Organ Transplantation:
- Individuals who have undergone organ transplantation and are on immunosuppressive medications have an increased risk of Herpes Zoster.
- Immunosuppression is necessary to prevent organ rejection but can lead to viral reactivation.
7. Radiation or Chemotherapy:
- Cancer treatments such as radiation therapy or chemotherapy can weaken the immune system, increasing the risk of shingles.
- These therapies may also directly damage nerve tissue, facilitating viral reactivation.
8. Family History:
- There may be a genetic predisposition to developing Herpes Zoster, although the exact mechanisms are not fully understood.
- A family history of shingles may indicate an increased risk for individuals.
9. Gender:
- Studies suggest that women may be slightly more likely to develop shingles compared to men.
- Hormonal changes, particularly during menopause, may contribute to this difference in risk.
10. Trauma or Injury:
- Physical trauma or injury to the skin can disrupt nerve function and increase the likelihood of Herpes Zoster in the affected area.
- Surgical procedures or accidents that damage nerves may trigger viral reactivation.
Treatment of Shingles:
1. Antiviral Medications:
- Antiviral drugs such as acyclovir, valacyclovir, and famciclovir are commonly prescribed to reduce the severity and duration of shingles symptoms.
- These medications work by inhibiting the replication of the varicella-zoster virus, speeding up the healing process and reducing the risk of complications.
2. Pain Management:
- Pain management is a crucial aspect of shingles treatment, especially since pain can persist even after the rash has healed.
- Over-the-counter pain relievers such as acetaminophen or ibuprofen may help alleviate mild to moderate pain.
- For severe pain, prescription medications such as opioids or anticonvulsants may be prescribed.
3. Topical Treatments:
- Calamine lotion or colloidal oatmeal baths can help soothe itching and discomfort associated with shingles blisters.
- Topical creams or gels containing capsaicin, lidocaine, or numbing agents may also provide relief from pain and itching.
4. Corticosteroids:
- In some cases, corticosteroids may be prescribed to reduce inflammation and swelling associated with Herpes Zoster.
- Oral corticosteroids such as prednisone may be used in combination with antiviral medications for severe cases or to prevent complications such as postherpetic neuralgia.
5. Antidepressants and Anticonvulsants:
- Certain antidepressant medications, such as tricyclic antidepressants or selective serotonin reuptake inhibitors (SSRIs), may be prescribed to help manage nerve-related pain.
- Anticonvulsant drugs such as gabapentin or pregabalin may also be effective in reducing nerve pain associated with Herpes Zoster.
6. Cool Compresses:
- Applying cool compresses or ice packs to the affected area can help relieve pain and reduce inflammation.
- It’s essential to avoid direct contact between ice and the skin to prevent further irritation or damage.
7. Rest and Comfort:
- Getting plenty of rest and avoiding activities that aggravate pain or discomfort can promote healing and recovery.
- Wearing loose-fitting clothing and avoiding tight or restrictive garments can help minimize irritation to the rash.
8. Eye Care:
- If shingles affect the eyes (herpes zoster ophthalmicus), prompt treatment is essential to prevent complications such as vision loss.
- Antiviral eye drops or ointments may be prescribed, along with oral antiviral medications and corticosteroid eye drops to reduce inflammation.
9. Vaccination:
- The shingles vaccine (Shingrix) is recommended for adults aged 50 and older to prevent shingles and reduce the risk of complications.
- Vaccination is particularly important for individuals at higher risk of developing shingles, such as those with weakened immune systems or a history of chickenpox.
10. Follow-Up Care:
- Regular follow-up appointments with a healthcare provider are essential to monitor the progress of shingles treatment and address any complications or lingering symptoms.
- It’s crucial to seek medical attention promptly if new symptoms develop or existing symptoms worsen during the course of treatment.
Complications:
While typically it resolves within two to four weeks with proper treatment, complications can arise, particularly in older adults and individuals with weakened immune systems. Postherpetic neuralgia, characterized by persistent pain in the affected area, is one of the most common complications of shingles. Other potential complications include bacterial skin infections, eye complications such as keratitis or vision loss, and neurological problems such as facial paralysis or encephalitis.
Conclusion
In conclusion, it is a painful and potentially debilitating condition caused by the reactivation of the varicella-zoster virus. Understanding its causes, symptoms, treatment, and potential complications is essential for effective management and prevention of long-term health issues. Early diagnosis and prompt treatment with antiviral medications can shorten the duration of the rash, alleviate pain, and reduce the risk of complications. Additionally, vaccination against it with the herpes zoster vaccine can help prevent the development of shingles or reduce its severity in individuals who do contract the virus. By raising awareness and taking proactive measures, individuals can minimize the impact of shingles on their health and well-being.
Frequently Asked Questions (FAQs) on Shingles
1. What is the main cause of shingles?
- Shingles is caused by the reactivation of the varicella-zoster virus, the same virus responsible for chickenpox, which remains dormant in nerve tissue after initial infection.
2. How long will shingles last?
- The duration of Herpes Zoster varies, but the rash typically lasts 2 to 4 weeks. Pain may persist even after the rash has healed, especially in cases of postherpetic neuralgia.
3. Is shingles a serious problem?
- Shingles can be a serious problem, especially in older adults or individuals with weakened immune systems. Complications such as postherpetic neuralgia, nerve damage, or eye involvement can occur.
4. What deficiency causes shingles?
- Shingles is not directly caused by a specific nutrient deficiency. However, a weakened immune system due to factors such as malnutrition or certain medical conditions may increase the risk of Herpes Zoster.
5. Who is at risk for shingles?
- Older adults, individuals with weakened immune systems, those who have had chickenpox, and people under significant stress are at higher risk of developing Herpes Zoster.
6. Is shingles caused by stress?
- While stress does not directly cause shingles, it can weaken the immune system, making individuals more susceptible to viral reactivation and the development of Herpes Zoster.
7. How to cure shingles quickly?
- There is no cure for Herpes Zoster, but antiviral medications can help reduce the severity and duration of symptoms if started early. Pain management, rest, and supportive care can also aid in recovery.
8. What is the best treatment for shingles?
- Treatment for Herpes Zoster typically involves antiviral medications, pain management, and supportive care to alleviate symptoms and promote healing. Consultation with a healthcare provider is essential for personalized treatment.
9. How to sleep with shingles?
- Sleeping with Herpes Zoster can be challenging due to pain and discomfort. Using soft bedding, applying cool compresses to affected areas, and taking pain medication before bedtime may help improve sleep quality.
10. How to cure shingles in 3 days?
- While there is no guaranteed way to cure shingles in 3 days, starting antiviral medication early and following treatment recommendations from a healthcare provider may help accelerate recovery and reduce symptom duration.
11. What is the most painful stage of shingles?
- The most painful stage of shingles is often during the active phase of the rash, when blisters are present. Pain may persist even after the rash has healed, especially in cases of postherpetic neuralgia.

Pingback: Milroy's Disease: Causes, Symptoms, Treatment, and Complications - Modern Health
Pingback: Common Health Conditions - Modern Health