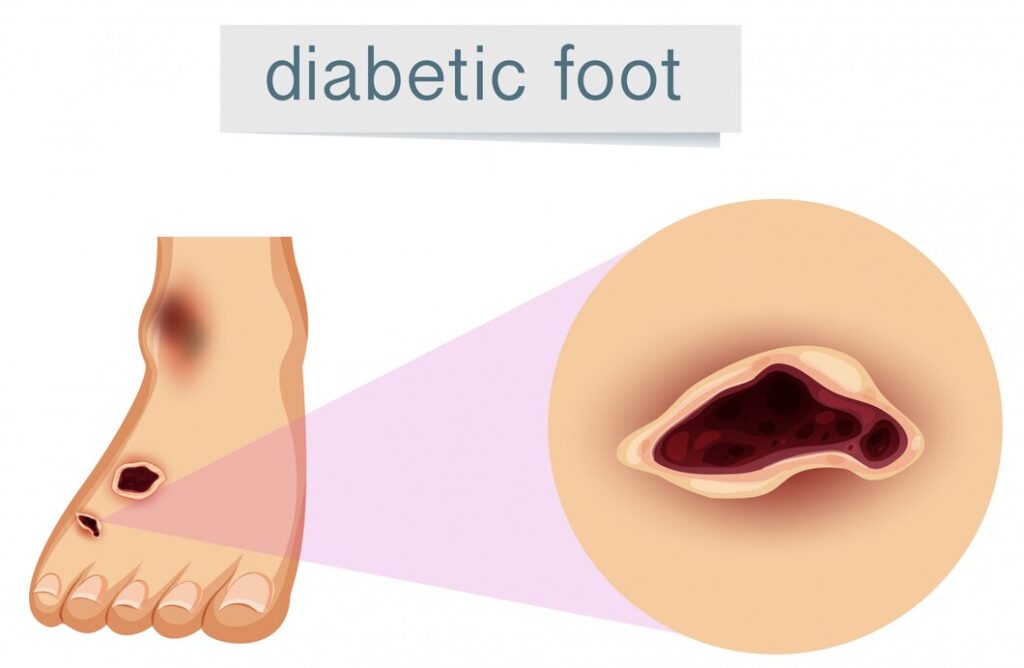
Diabetic foot ulcer;
Overview:
Diabetic foot ulcer, a common complication of diabetes mellitus, poses significant challenges for individuals living with the condition.
What is Diabetic Foot ulcer?
Diabetic foot refers to a spectrum of foot problems that occur in individuals with diabetes due to nerve damage (neuropathy) and poor circulation (vascular disease). It encompasses a range of conditions, including ulcers, infections, and deformities, which can lead to serious complications if left untreated.
Mechanism And Risk Factors of Diabetic Foot Ulcer:
Diabetic foot ulcer result from a complex interplay of various factors inherent to diabetes mellitus.
1. Peripheral Neuropathy
Peripheral neuropathy, a common complication of diabetes, lies at the core of diabetic foot ulcers. Here’s how it unfolds:
- Nerve Damage: Elevated blood sugar levels over time lead to nerve damage, impairing sensation in the feet.
- Sensory Loss: Individuals with diabetic neuropathy may experience numbness, tingling, or loss of feeling in their feet.
- Unnoticed Injuries: Reduced sensation makes it difficult to detect injuries, allowing wounds to go unnoticed and untreated.
2. Reduced Blood Flow
Peripheral vascular disease, often accompanying diabetes, exacerbates the risk of foot ulcers.
- Impaired Circulation: Diabetes damages blood vessels, reducing blood flow to the feet.
- Oxygen and Nutrient Deficiency: Diminished circulation hinders the delivery of oxygen and nutrients to the tissues, impeding wound healing.
- Increased Vulnerability: Poor circulation makes individuals with diabetes more susceptible to ulcer formation and delayed wound healing.
3. Foot Deformities and Pressure Points
Foot deformities contribute significantly to the development of diabetic foot ulcers. Consider the following:
- Altered Pressure Distribution: Deformities like bunions and hammertoes alter the distribution of pressure on the feet.
- Excessive Friction: Irregular pressure points result in excessive rubbing and friction, predisposing to calluses, blisters, and ulcers.
- Common Sites: Bony prominences and pressure points are particularly prone to ulcer formation due to repetitive trauma.
4. Impaired Immune Function
Diabetes compromises the immune system, increasing the risk of infections in foot wounds.
- Elevated Blood Sugar: High blood sugar levels create a favorable environment for bacterial growth in wounds.
- Heightened Infection Risk: Impaired immune function increases susceptibility to infections in foot ulcers.
- Complications: Infections can exacerbate tissue damage, delay wound healing, and lead to serious complications like cellulitis or osteomyelitis.
5. Compromised Wound Healing
Chronic inflammation plays a pivotal role in the delayed healing of diabetic foot ulcers. Here’s how it leads:
- Persistent Inflammation: Elevated levels of pro-inflammatory cytokines disrupt the normal wound healing process.
- Impaired Regeneration: Dysregulated signaling pathways impede cell proliferation and tissue regeneration.
- Chronicity: Prolonged inflammation contributes to the chronic nature of diabetic foot ulcers, necessitating targeted anti-inflammatory interventions.
Signs and Symptoms:
Diabetic foot ulcers are a serious complication of diabetes mellitus, characterized by non-healing wounds on the feet.
1. Persistent Wounds
- Open Sores: Diabetic foot ulcers typically present as open sores or wounds on the feet, often located on the bottom of the foot or over bony prominences.
- Slow Healing: These wounds may persist for weeks or even months without showing signs of improvement, despite appropriate wound care measures.
- Recurrence: Diabetic foot ulcers have a tendency to recur, especially if underlying risk factors such as neuropathy or poor circulation are not addressed.
2. Skin Changes
- Redness or Swelling: The skin surrounding the ulcer may appear red, swollen, or inflamed, indicating an inflammatory response to the wound.
- Warmth: The affected area may feel warmer to the touch compared to the surrounding skin due to increased blood flow and inflammation.
- Discoloration: Changes in skin color, ranging from pink to deep red or even purple, may be observed around the ulcer site.
3. Drainage or Odor
- Drainage: Diabetic foot ulcers may produce pus or other types of discharge, indicating the presence of infection.
- Foul Odor: The wound may emit a foul odor, particularly if infection is present, due to the breakdown of tissue and bacterial proliferation.
4. Pain or Discomfort
- Pain Sensation: Although neuropathy can diminish sensation in the feet, some individuals may experience pain or discomfort, especially if the ulcer is infected or if there is pressure on the wound site.
- Pain Relief: Pain relief may occur temporarily if nerve damage is severe, leading to decreased sensation in the affected area.
5. Complications
- Cellulitis: If left untreated, diabetic foot ulcers can progress to cellulitis, a bacterial skin infection characterized by redness, warmth, and tenderness in the affected area.
- Osteomyelitis: In severe cases, the infection may spread to the underlying bone, resulting in osteomyelitis, which requires prompt medical attention and may necessitate surgical intervention.
Prevention:
Preventing diabetic foot complications begins with proactive foot care and regular monitoring. Individuals with diabetes should inspect their feet daily for cuts, blisters, or signs of infection and seek prompt medical attention for any abnormalities. Proper foot hygiene, wearing comfortable shoes, and maintaining optimal blood sugar levels are essential for preventing complications.
Treatment :
Diabetic foot ulcers demand prompt and comprehensive treatment to prevent complications and promote healing.
1. Wound Debridement
- Removal of Dead Tissue: Debridement involves removing necrotic or dead tissue from the ulcer site to facilitate wound healing.
- Enhancing Healing: By eliminating non-viable tissue, debridement promotes the growth of healthy tissue and reduces the risk of infection.
- Methods: Debridement techniques may include sharp debridement (using surgical instruments), enzymatic debridement (using topical enzymes), mechanical debridement (using wet-to-dry dressings), or autolytic debridement (using moist dressings to allow the body’s natural enzymes to break down dead tissue).
2. Infection Management
- Antibiotic Therapy: If infection is present or suspected, antibiotic therapy may be initiated to control bacterial growth and prevent systemic spread.
- Cultures: Wound cultures may be obtained to identify the specific bacteria causing the infection and guide antibiotic selection for targeted therapy.
- Surgical Intervention: In severe cases of infection or osteomyelitis (bone infection), surgical debridement or drainage may be necessary to remove infected tissue and promote healing.
3. Offloading Pressure
- Redistribution of Pressure: Offloading pressure from the ulcer site is essential to prevent further tissue damage and promote healing.
- Orthotic Devices: Customized footwear, orthotic inserts, or special braces may be prescribed to redistribute pressure and reduce stress on the affected foot.
- Avoidance of Weight-Bearing: Patients may be advised to minimize weight-bearing activities or use assistive devices such as crutches or walkers to offload pressure from the foot during the healing process.
4. Moist Wound Healing
- Moist Dressings: Keeping the wound moist with appropriate dressings creates an optimal environment for healing by promoting cell migration, angiogenesis, and granulation tissue formation.
- Hydrogels, foams, hydrocolloids, and alginates are examples of moisture-retentive dressings commonly used in the management of diabetic foot ulcers.
5. Blood Glucose Control
- Tight Glycemic Control: Maintaining optimal blood glucose levels is essential for promoting wound healing and preventing complications.
- Collaboration with Healthcare Team: Patients with diabetes should work closely with their healthcare providers to optimize blood sugar control through medication adjustments, dietary modifications, and regular monitoring.
6. Advanced Therapies
- Growth Factors: Growth factor therapy involves the application of bioactive proteins to stimulate tissue repair and accelerate wound healing.
- Negative Pressure Wound Therapy (NPWT): NPWT utilizes negative pressure to promote wound healing by reducing edema, enhancing blood flow, and removing excess exudate.
- Hyperbaric Oxygen Therapy (HBOT): HBOT involves the administration of 100% oxygen in a pressurized chamber, which increases oxygen delivery to tissues and promotes healing in chronic wounds, including diabetic foot ulcers.
7. Patient Education and Self-Care
- Foot Care Education: Patients should receive comprehensive education on foot care practices, including daily inspection of the feet, proper hygiene, appropriate footwear selection, and early recognition of signs of infection or injury.
Lifestyle Modifications:
In addition to medical interventions, lifestyle modifications play a crucial role in managing diabetic foot. Maintaining a healthy weight, following a balanced diet, engaging in regular physical activity, and avoiding tobacco and excessive alcohol consumption can improve overall foot health and reduce the risk of complications.
Summary:
Diabetic foot presents significant challenges for individuals with diabetes, but with proactive management and proper foot care, many complications can be prevented.
Read Another Article: Health Benefits of Ashwagandha