Babesia;
Introduction
Babesiosis is a tick-borne disease caused by microscopic parasites that infect red blood cells. This disease can range from mild to severe and can even be life-threatening, especially in individuals with weakened immune systems. Babesiosis is primarily transmitted through the bite of an infected tick, but it can also be spread through blood transfusions or from mother to baby during pregnancy.
Case Presentation
A 45-year-old woman visited her doctor with complaints of fever, chills, muscle aches, and fatigue. She had recently returned from a hiking trip in a region known for high tick activity. Upon physical examination, her spleen was slightly enlarged, and her blood tests revealed anemia. Further laboratory tests, including a blood smear and polymerase chain reaction (PCR) testing, confirmed the presence of Babesia parasites in her red blood cells, diagnosing her with babesiosis.
Overview
What is Babesiosis?
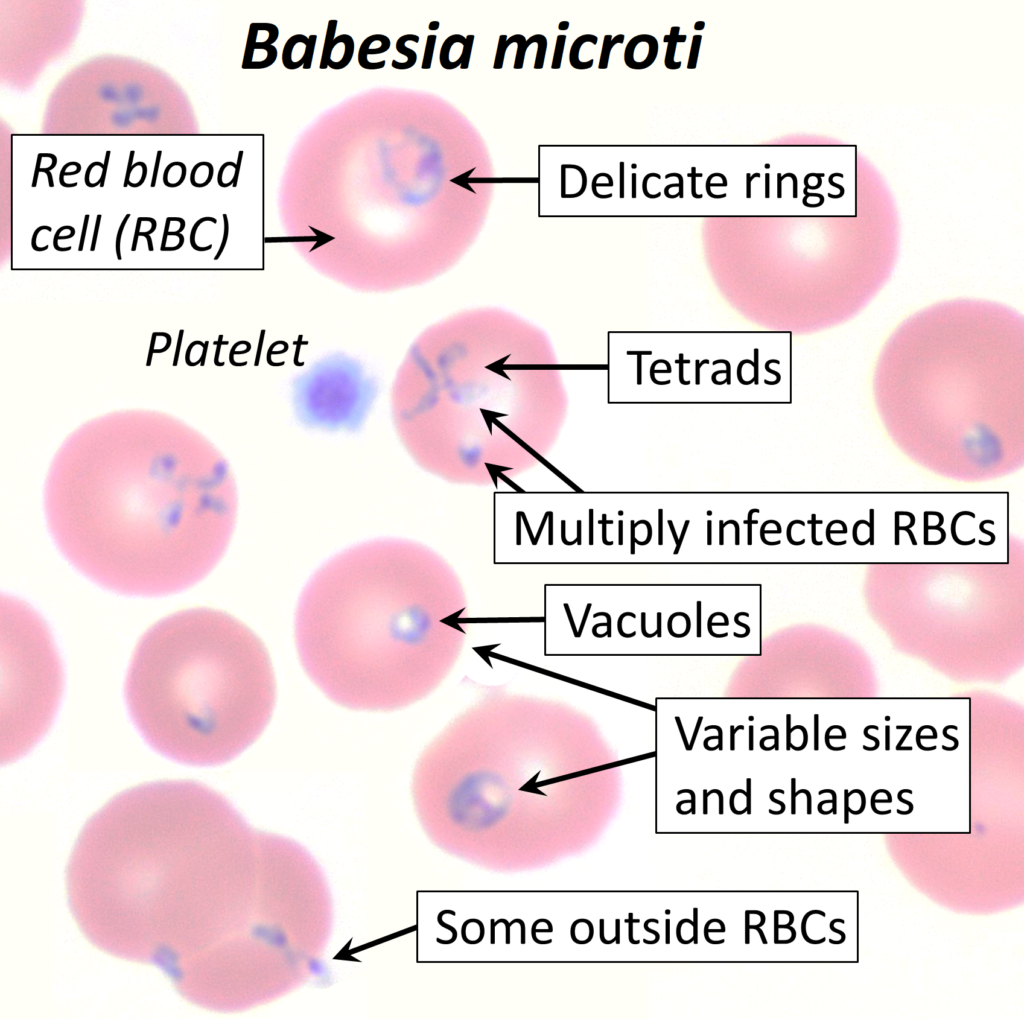
Babesiosis is an infection caused by protozoan parasites of the genus Babesia, which infect and destroy red blood cells. The disease is similar to malaria in terms of its effects on red blood cells but is caused by a different group of parasites.
Where is it Found?
Babesiosis is most commonly found in:
- Northeastern and upper Midwestern United States: Particularly in states like New York, New Jersey, Wisconsin, and Minnesota.
- Parts of Europe: Such as Ireland, the United Kingdom, and other areas with high deer populations.
- Some tropical and subtropical areas: Though less common, babesiosis can also occur in regions where tick populations are prevalent.
How Do People Get It?
Babesiosis is primarily transmitted through the bite of infected black-legged ticks (Ixodes scapularis), also known as deer ticks. These ticks are often found in grassy, wooded, or brushy areas, making outdoor activities in these environments a risk factor for infection. Less commonly, babesiosis can be transmitted through:
- Blood transfusions: Receiving blood from an infected donor.
- Congenital transmission: From an infected mother to her baby during pregnancy.
Symptoms of Babesiosis
Common Symptoms
Symptoms of babesiosis can vary widely and may resemble those of other tick-borne diseases or viral infections. Common symptoms include:
- Fever: Often high and can come and go.
- Chills: Accompanying the fever.
- Sweats: Profuse sweating, particularly at night.
- Headache: Persistent and severe.
- Body aches and muscle pain: Generalized pain in muscles and joints.
- Loss of appetite: Decreased desire to eat.
- Nausea: Feeling of wanting to vomit.
- Fatigue: Extreme tiredness and lack of energy.
Severe Symptoms
In some cases, especially among individuals with weakened immune systems, the elderly, or those without a spleen (asplenia), babesiosis can cause severe and life-threatening symptoms, such as:
- Severe anemia: Due to the destruction of red blood cells.
- Organ failure: In severe cases, organs such as the liver, kidneys, and lungs may fail.
- Difficulty breathing: Due to severe anemia or lung involvement.
- Low blood pressure: Which can lead to shock.
Diagnosis
How is it Diagnosed?
Diagnosing babesiosis can be challenging because its symptoms are similar to those of other illnesses. However, several methods can confirm the infection:
- Blood Smear: A drop of blood is examined under a microscope to look for the presence of Babesia parasites inside red blood cells.
- PCR Testing: This method detects Babesia DNA in the blood and is very sensitive.
- Serology: Blood tests to detect antibodies against Babesia. This method can indicate a current or past infection.
- Complete Blood Count (CBC): To check for anemia and other abnormalities in blood cells.
Treatment
Medications
Treatment for babesiosis typically involves a combination of medications. The most common regimen includes:
- Atovaquone: An anti-parasitic medication.
- Dose: 750 mg orally every 12 hours for 7-10 days.
- Azithromycin: An antibiotic.
- Dose: 500-1000 mg on the first day, followed by 250 mg orally once daily for 7-10 days.
For more severe cases, an alternative combination may be used:
- Clindamycin: An antibiotic.
- Dose: 600 mg intravenously every 6 hours, or 300-600 mg orally every 6-8 hours.
- Quinine: An anti-malarial drug.
- Dose: 650 mg orally every 6-8 hours for 7-10 days.
Supportive Care
In severe cases of babesiosis, additional supportive care may be necessary:
- Blood Transfusions: To treat severe anemia.
- Hospitalization: For monitoring and managing complications such as organ failure or severe respiratory issues.
Prevention
Avoid Tick Bites
Preventing tick bites is crucial in reducing the risk of babesiosis. Effective strategies include:
- Wear Protective Clothing: Long sleeves, long pants, and hats can help protect your skin from ticks.
- Use Insect Repellent: Products containing DEET, picaridin, or permethrin can repel ticks.
- Stay on Trails: Avoid walking through tall grass and brush where ticks are common.
Tick Checks
After spending time outdoors, especially in tick-infested areas:
- Perform Tick Checks: Thoroughly check your body, clothing, and pets for ticks.
- Shower Soon After: Showering within two hours of being outdoors can help remove ticks before they attach.
- Remove Ticks Properly: Use fine-tipped tweezers to grasp the tick as close to the skin as possible and pull upward with steady pressure.
Tick Control
Managing the tick population around your home can also help prevent babesiosis:
- Keep Grass Short: Regularly mow your lawn to reduce tick habitat.
- Remove Leaf Litter: Clear leaves and brush from your yard.
- Use Tick Control Products on Pets: Protect your pets with tick prevention products.
Conclusion
Babesiosis is a serious tick-borne illness that can cause a range of symptoms from mild to severe. Prompt diagnosis and treatment are essential for managing the disease effectively. Preventing tick bites through protective measures and environmental management is the best way to reduce the risk of infection.
Read more:

