Tinea versicolor;
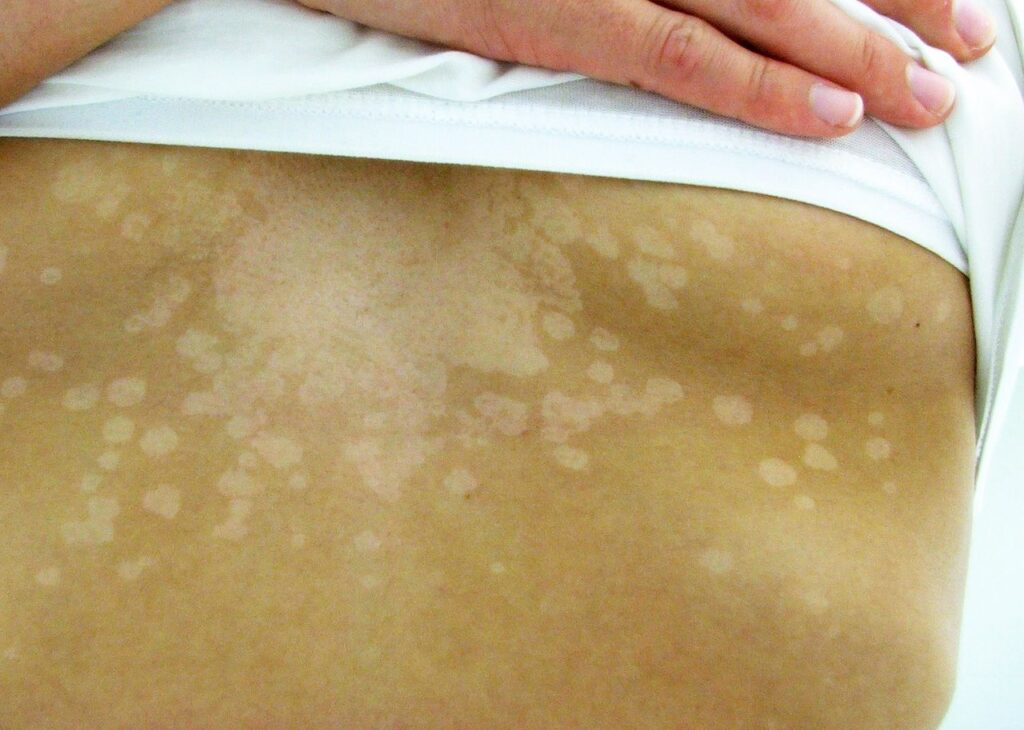
What is Tinea Versicolor?
Tinea versicolor, also known as pityriasis versicolor, is a common fungal infection of the skin. It is caused by the overgrowth of a type of yeast called Malassezia, which normally resides on the skin without causing any harm. However, under certain conditions, such as warm and humid environments, excessive sweating, or weakened immune system, Malassezia can proliferate and lead to the development of pityriasis versicolor.
Causes of Tinea Versicolor
The primary cause of pityriasis versicolor is the overgrowth of the yeast Malassezia on the skin. This overgrowth can be triggered by various factors, including:
- Humid and warm weather conditions
- Excessive sweating
- Oily skin
- Weakened immune system
- Hormonal changes, such as those occurring during puberty or pregnancy
Risk Factors for Tinea Versicolor
Several factors may increase an individual’s risk of developing pityriasis versicolor, including:
- Climate: Living in warm and humid climates increases the risk of pityriasis versicolor due to favorable conditions for yeast growth.
- Excessive Sweating: People who sweat excessively, either due to physical activity or certain medical conditions, are more prone to developing Pityriasis versicolor.
- Oily Skin: Individuals with naturally oily skin have a higher risk of developing pityriasis versicolor as the excess oil provides a suitable environment for yeast growth.
- Weakened Immune System: Conditions that weaken the immune system, such as HIV/AIDS or immunosuppressive medications, increase the risk of fungal infections, including pityriasis versicolor.
Symptoms of Tinea Versicolor:
The symptoms of pityriasis versicolor can vary but often include:
- Patches: Small, discolored patches of skin, usually lighter or darker than the surrounding skin.
- Scaling: Fine, flaky scales on the affected areas of the skin.
- Itching: Mild to moderate itching may occur, especially in warm conditions or after sweating.
- Changes in Skin Color: The patches may become more noticeable after sun exposure due to the lack of pigmentation in affected areas.
Differential Diagnosis of Tinea Versicolor:
When encountering skin conditions, it’s crucial for dermatologists to consider a range of potential diagnoses to accurately identify the underlying cause. Tinea versicolor, although distinct in its presentation, shares similarities with other skin conditions, making a thorough differential diagnosis essential for proper management.
Differential Diagnosis:
1. Pityriasis Rosea
- Presentation: Pityriasis rosea often begins with a single, large, scaly patch known as a herald patch, followed by smaller, oval-shaped lesions spreading across the trunk and limbs.
- Distinguishing Features: Unlike tinea versicolor, pityriasis rosea lesions typically follow a distinct pattern along the skin’s lines of cleavage (the so-called “Christmas tree” distribution), and the scales are often finer.
2. Seborrheic Dermatitis
- Presentation: Seborrheic dermatitis presents with red, greasy, scaly patches, commonly affecting areas rich in sebaceous glands, such as the scalp, face, and chest.
- Distinguishing Features: While seborrheic dermatitis shares a similar appearance with tinea versicolor, it tends to involve areas with higher concentrations of sebaceous glands, and the scales may appear yellowish rather than white.
3. Vitiligo
- Presentation: Vitiligo is characterized by depigmented, well-defined patches of skin, which may vary in size and shape.
- Distinguishing Features: Unlike tinea versicolor, which typically presents with hypo- or hyperpigmented patches, vitiligo results in complete loss of pigmentation in affected areas, often with sharp borders.
4. Post-inflammatory Hypopigmentation
- Presentation: Post-inflammatory hypopigmentation can result from various skin conditions, injuries, or inflammatory reactions, leading to patches of lighter skin.
- Distinguishing Features: Unlike tinea versicolor, which is caused by a fungal infection, post-inflammatory hypopigmentation occurs as a result of trauma or inflammation and may not exhibit scales or other fungal characteristics.
How to Diagnose pityriasis versicolor?
In addition to clinical presentation, several diagnostic tools and tests may aid in the differential diagnosis of tinea versicolor:
- Wood’s Lamp Examination: Wood’s lamp examination can help visualize fungal elements fluorescing under ultraviolet light, aiding in the diagnosis of pityriasis versicolor.
- KOH (Potassium Hydroxide) Preparation: Microscopic examination of skin scrapings treated with KOH can reveal fungal hyphae and spores, supporting the diagnosis of tinea versicolor.
- Skin Biopsy: In cases where the diagnosis is uncertain, a skin biopsy may be performed to examine tissue samples under a microscope, helping to differentiate pityriasis versicolor from other skin conditions.
Distinguishing pityriasis versicolor from other skin conditions is essential for appropriate management and treatment.
Treatment :
Treatment for pityriasis versicolor typically involves the use of antifungal medications, which can be applied topically or taken orally, depending on the severity of the infection. Common treatments include:
- Topical Antifungals: Creams, lotions, or shampoos containing antifungal agents such as ketoconazole, selenium sulfide, or ciclopirox are often prescribed for mild to moderate cases of pityriasis versicolor.
- Oral Antifungals: In cases of severe or widespread infection, oral antifungal medications such as fluconazole or itraconazole may be prescribed by a healthcare professional.
- Maintenance Therapy: To prevent recurrence, periodic use of antifungal shampoos or creams may be recommended, especially for individuals prone to recurrent infections.
Prevention:
While pityriasis versicolor is not always preventable, certain measures can help reduce the risk of developing the infection:
- Maintain Good Hygiene: Regularly showering and keeping the skin clean can help prevent the buildup of sweat and oil, which can contribute to yeast overgrowth.
- Avoid Excessive Heat and Humidity: Limit exposure to hot and humid environments, and wear loose-fitting clothing made of breathable fabrics.
- Use Antifungal Products: For individuals prone to pityriasis versicolor, using antifungal shampoos or creams regularly may help prevent recurrence.
- Limit Sun Exposure: Avoid prolonged sun exposure, especially during peak hours, as UV radiation can exacerbate pityriasis versicolor symptoms.
By understanding the causes, risk factors, symptoms, treatment, and prevention of tinea versicolor, individuals can take proactive steps to manage this common fungal infection and maintain healthy skin.

Very useful information
Pingback: Rosacea - causes , Treatment - Modern Health
Pingback: Ringworm(Tinea)- Causes And Treatment - Modern Health
Pingback: Pityriasis Rosea: cause, symptoms, Treatment - Modern HealthMe