Cutaneous larva migrans;
Introduction
Cutaneous larva migrans (CLM) is a parasitic skin infection caused by the larvae of animal hookworms, predominantly the Ancylostoma braziliense and Ancylostoma caninum species. This condition commonly affects individuals who have been in contact with contaminated soil or sand in tropical and subtropical regions.
Causes of Cutaneous larva migrans (CLM):
When human skin comes into contact with these larvae-infested environments, the larvae can penetrate the skin, leading to infection.
Causes:
1. Parasitic Origin
- Hookworm Infection (Ancylostoma braziliense or Ancylostoma caninum): The larvae of these hookworm species, found in the feces of infected dogs and cats, penetrate human skin, leading to cutaneous larva migrans.
2. Environmental Factors
- Warm and Moist Climates: CLM is more prevalent in tropical and subtropical regions due to the favorable environmental conditions for parasite survival and development.
3. Human Behavior
- Barefoot Walking: Walking barefoot on contaminated soil or sand increases the risk of larvae penetrating the skin, especially in areas where animals commonly defecate.
4. Outdoor Activities
- Beach Activities: Engaging in activities such as sunbathing, playing in sand, or walking along beaches where contaminated soil is present can expose individuals to infective larvae.
5. Poor Sanitation
- Lack of Animal Waste Management: In areas with inadequate waste disposal systems for animal feces, contaminated environments become breeding grounds for parasites, heightening the risk of transmission to humans.
6. Limited Awareness
- Lack of Knowledge: Insufficient awareness about the risks associated with walking barefoot in contaminated areas or neglecting personal hygiene practices can contribute to the spread of cutaneous larva migrans.
Read Another Article: Rocky Mountain Spotted Fever
What Is Rocky Mountain Spotted Fever(RMSF)
Mechanism of cutaneous larva migrans:
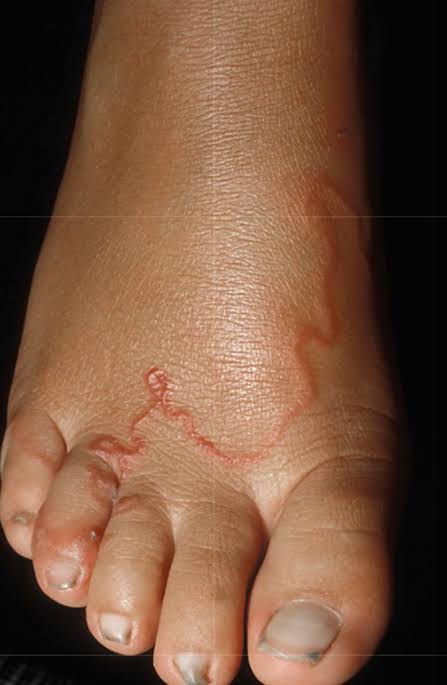
Upon penetrating the skin, hookworm larvae migrate through the epidermis, causing characteristic serpiginous tracks. The larvae do not mature into adult worms in humans but instead wander beneath the skin, causing inflammation and itching. As they move, they leave a trail of allergic reaction and tissue destruction, resulting in the characteristic winding rash seen in CLM.
Symptoms:
1. Skin Manifestations
- Linear or Serpiginous Lesions: The hallmark symptom of CLM is the appearance of winding, raised, red-to-pink tracks on the skin, typically measuring a few millimeters to centimeters in length.
- Pruritus (Itching): Intense itching often accompanies the lesions, leading to discomfort and scratching.
2. Migration Patterns
- Slow Progression: The lesions may exhibit slow, erratic migration over the skin surface, as the larvae move beneath the epidermis.
3. Secondary Infections
- Bacterial Superinfection: Due to scratching and compromised skin integrity, secondary bacterial infections may develop, leading to symptoms such as increased redness, swelling, warmth, and pus formation.
4. Duration and Persistence
- Chronicity: Cutaneous larva migrans lesions can persist for weeks to months if left untreated, with new lesions potentially developing as existing ones heal.
5. Systemic Symptoms
- Rare: Systemic symptoms are rare in cutaneous larva migrans but may occur in severe cases or with secondary infections, presenting as fever, malaise, or regional lymphadenopathy.
Risk Factors
Individuals at higher risk of developing CLM include those who frequent beaches, sandboxes, or other areas with contaminated soil. Activities such as walking barefoot or sitting directly on the ground increase the risk of skin exposure to hookworm larvae, particularly Ancylostoma braziliense and Ancylostoma caninum species. Travel to tropical or subtropical regions where CLM is endemic also elevates the risk.
Treatment of cutaneous larva migrans
1. Topical Therapies
- Antiparasitic Creams or Lotions: Topical application of antiparasitic medications such as thiabendazole or albendazole can effectively kill the larvae and alleviate symptoms. These medications are usually applied directly to the affected areas once or twice daily for 1 to 7 days, depending on the severity of the infestation.
- Corticosteroid Creams: In cases of intense itching and inflammation, topical corticosteroid creams may be prescribed to reduce itching and promote healing. However, they are typically used in combination with antiparasitic medications and for a limited duration to avoid complications.
2. Oral Medications
- Antiparasitic Drugs: In severe or widespread cases of cutaneous larva migrans, oral antiparasitic medications such as albendazole or ivermectin may be prescribed. These drugs work systemically to kill the larvae throughout the body and are typically administered as a single dose or a short course of treatment.
3. Symptomatic Relief
- Antihistamines: Oral antihistamines may be recommended to alleviate itching and reduce the inflammatory response associated with cutaneous larva migrans lesions. They can help improve the patient’s comfort and quality of life during treatment.
4. Prevention of Secondary Infections
- Topical or Oral Antibiotics: If secondary bacterial infections develop due to scratching and compromised skin integrity, topical or oral antibiotics may be prescribed to treat the infection and prevent complications.
5. Patient Education
- Hygiene and Prevention Measures: Patients should be educated about the importance of maintaining good hygiene practices, avoiding walking barefoot in contaminated areas, and wearing protective footwear when outdoors to prevent reinfestation.
Summary:
Cutaneous larva migrans, caused primarily by Ancylostoma braziliense and Ancylostoma caninum species, is a parasitic skin infection prevalent in tropical and subtropical regions.
Read Another Article – Health Benefits of Ashwagandha

Nice
Pingback: Home - Common health conditions - ECG Oxford
Pingback: common health conditions - Health Google